Tag: diabetes

The time is now for stewardship in diabetic foot infections
Diabetes, first described in ancient Egypt, remains at the forefront of health care in modern times. Roughly 537 million adults aged 20 to 79 years are living with diabetes worldwide, a number expected to rise over the next decades … Diabetic complications are vast. Diabetic foot infection (DFI) is a chronic, more severe complication that affects roughly 15% of people with diabetes. DFIs have been associated with decreased quality of life, frequent and prolonged hospitalizations and greater risk for lower extremity amputation … read more
We Are Failing Our Patients With Diabetes
My career in medicine has spanned approximately 26 years. Nineteen-ninety-six was my first year of residency training as well as my first real exposure to the emerging specialty of wound care.
To put things into perspective, during my first year of training, there were approximately 300–500 wound care products on the market. That may seem like a lot, especially considering there are now thousands of products that wound providers and others may choose from. Consider, however, that when I began clinical practice, the resources available were considerably different when compared to what is available today … read more
The epidemic of diabetic limb amputation in poor communities and parts of Cleveland
Differences in outcomes across race, ethnicity and income exist for virtually every chronic health condition that Americans experience. Without exception, minority and poor white Americans die younger and suffer more preventable diseases.
November is diabetes awareness month. Few diseases impact every system of the body in the way that diabetes increases the risk for stroke, heart attack and kidney failure.
Of these devastating conditions, loss of limb, or amputation, is one of the most-dreaded complications of diabetes … read more
Healogics 8th Annual Diabetes Awareness Campaign, Chronic Wound Healing through Specialized Care
Healogics, the nation’s leading provider of world-class wound care services, is proud to announce the eighth annual Diabetes Awareness Campaign throughout the month of November, which is National Diabetes Awareness Month. The Healogics wound care specialists, at the more than 600 Healogics Wound Care Centers® nationwide, will be raising awareness of the importance of early intervention and specialized care for diabetes-related chronic wounds, such as diabetic foot ulcers … Diabetic foot ulcers are a leading cause of lower-limb amputations and according to the American Diabetes Association, an average of 10 Americans will undergo an amputation due to diabetes every hour. Of the 34.2 million Americans currently living with diabetes, up to 25% may develop a diabetic foot ulcer. These hard-to-heal wounds often go undetected due to the lack of feeling in the lower extremities due to nerve damage caused by diabetes … read more
Probiotics accelerate wound healing in patients with diabetic foot ulcer
Patients with diabetic foot ulcer (DFU) who were given probiotic supplements for 12 weeks had faster wound healing and improved glycemic control compared with similar patients on placebo, according to researchers who recently published their results in Diabetes/Metabolism Research and Reviews.
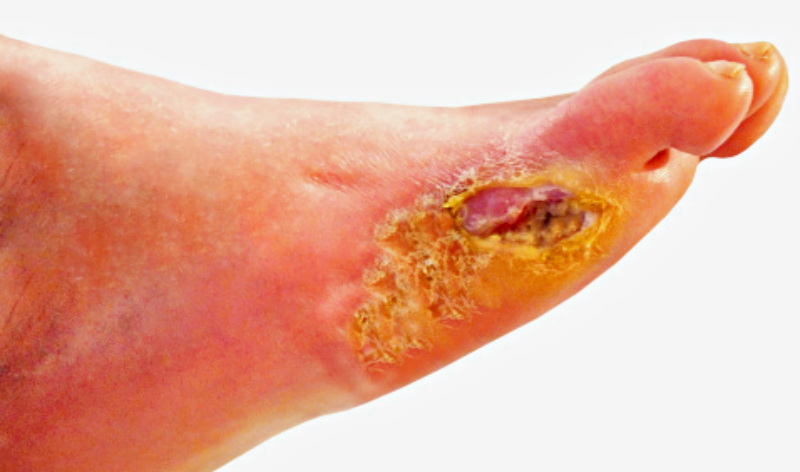
Diabetic foot ulcers healed faster in patients given probiotics.
“Due to the increasing global antimicrobial drug resistance issues, the idea of probiotic consumption is interesting and pertinent because probiotics have the ability to strengthen the immune system, have anti-inflammatory effects, and therefore, could increase the wound healing process,” wrote lead co-author Zatollah Asemi, PhD … read more
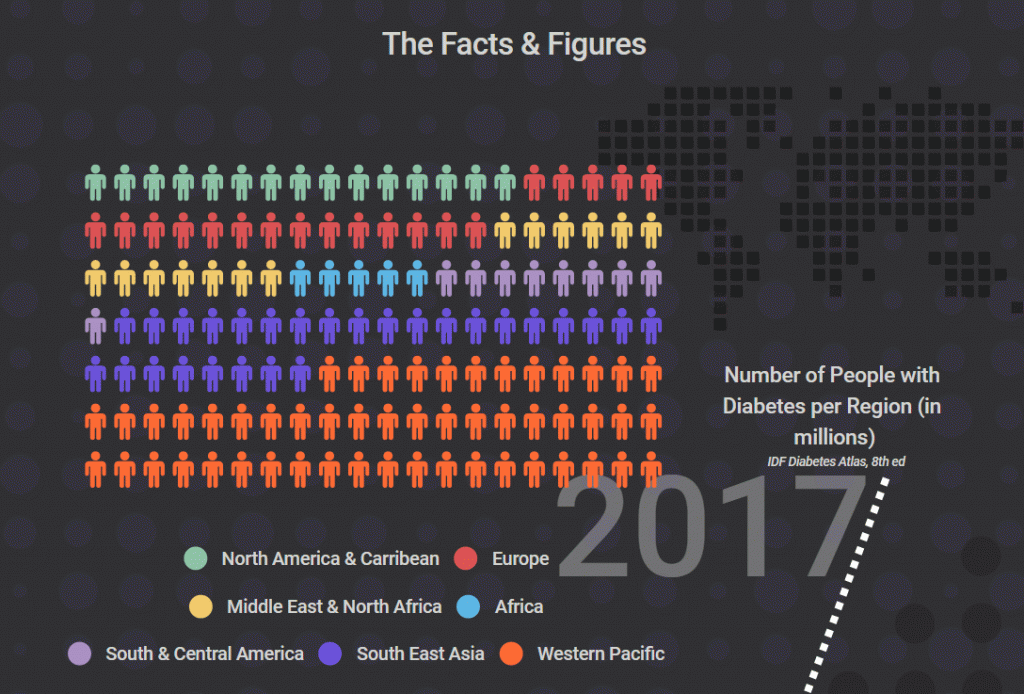
DIABETIC FOOT: FACTS AND FIGURES
A series of great informational graphics from Dr. Armstrong …. read more
1M diabetic people in Egypt at risk of amputation given hope by Sound Foot initiative
CAIRO – 4 October 2021: A total of L.E. 15 million have been allocated to support “Sound Foot” initiative to reduce the risks of diabetes, according to a Monday statement by the Ministry of Solidarity.
Some L.E.5 million of that budget will go to raising awareness on the diabetic foot and early detection. L.E. 10-15 million will go to treatment.
On Monday, Maker of Good Development, a charity organization that was established five years ago, held a conference to launch the initiative as part of the presidential initiative of Haya Karima. Minister of Solidarity Nivine el-Kabbag said in the conference that the Sound Foot initiative is a … read more
Footing the bill for diabetes
The world’s first Diabetic Foot Clinic was opened in 1981 at King’s College Hospital by Professor Michael Edmonds.
Since I jointly set up the Diabetic Foot Clinic at King’s College Hospital in 1981, I have seen how multidisciplinary care can have a huge impact on patient outcomes. Specialists working together under one roof can intervene and stop the progression of a disease which, if untreated, can swiftly lead on to tissue necrosis and gangrene. But, if I had to pick the one crucial thing that has really revolutionized our practice – helping to achieve a 50 percent reduction in major amputations … read more
Are Restaurants Exacerbating the Obesity Epidemic?
Since the COVID-19 pandemic began, almost all discussion of restaurant-related health has centered on one topic: how to protect diners and staff from the virus. But another health issue has been largely overlooked: how restaurants compromise Americans’ health by selling fare that is high in caloric density, fat, added sugars, and sodium, but low in essential fiber. And during a pandemic where obesity and other pre-existing health conditions have been risk factors for severe disease, this discussion couldn’t be more relevant.
It’s common knowledge that fast food sold by chains such as McDonald’s, Burger King, Wendy’s, and the like has a poor nutritional profile. But the appetizers, entrees, and desserts sold at full-service restaurants aren’t much better … read more
Foot Revascularization Avoids Major Amputation in Persons with Diabetes and Ischaemic Foot Ulcers
The study aims to evaluate the effectiveness of foot revascularization in persons with diabetic foot ulcers (DFUs) and below-the-ankle (BTA) arterial disease. Consecutive patients referred for a new active ischaemic DFU requiring lower limb revascularization were considered. Among those, only patients with a BTA arterial disease were included. Revascularization procedures were retrospectively analysed: in the case of successful foot revascularization (recanalization of pedal artery, or plantar arteries or both) or not, patients were respectively divided in two groups, successful foot perfusion (SFP) and failed foot perfusion (FFP). Healing, minor and major amputation at 12 months of follow-up were evaluated and compared. Eighty patients (80) were included. The mean age was 70.5 ± 10.9 years, 55 (68.7%) were male, 72 (90%) were affected by type 2 diabetes with a mean duration of 22.7 ± 11.3 years. Overall 45 (56.2%) patients healed, 47 (58.7%) had minor amputation and 13 (16.2%) major amputation. Outcomes for SFP and FFP were respectively: healing … read more
Rates of T1D-Related Amputations Decline in Sweden
Results of a Swedish retrospective cohort study showed reduced rates of type 1 diabetes-related amputations over the past 2 decades.
In recent years, Sweden has seen a sharp decline in incidence of lower-level extremity amputations among individuals with type 1 diabetes (T1D), according to results of an observational cohort study. Findings were published in Diabetologia.
Because diabetes-related foot ulcers are common and healing is often delayed, limb loss through amputation “is not an infrequent final outcome,” the authors explained.
In addition, “about half of all nontraumatic amputations in the western world are attributable to diabetes … read more
Combined Regenerative Approach for a Complex Lower Extremity Wound
More than 400 million patients worldwide are affected by diabetes; over their lifetime, at least 25% will develop foot ulcers that often result in high rates of nonhealing wounds and amputation. The authors present the case of a 43-year-old female patient with multiple comorbidities who presented with a large (8 cm x 4 cm), noninfected, hindfoot plantar ulcer that extended down to the bone and calcaneus. Over 2 weeks, the patient was successfully treated using a combination of an acellular dermal matrix, nanofat grafting, and negative pressure wound therapy, lessening the effects of the ulcer on the patient’s quality of life and achieving limb salvage. Utilizing the regenerative procedures described herein may improve patient care and decrease costs … read more
Study Shows Increased Risk For Foot Infection-Related Hospitalizations In People With Diabetes
According to a recent publication in Diabetologia, there is an increased risk of infection-related hospitalization in patients with diabetes.1 This includes foot infections, for which the risk of hospitalization was nearly six times greater in patients with diabetes than those without. Remarkably, the risk for hospitalization in patients with diabetes for all infection types, including foot infection, respiratory infection, urinary tract infection, GI infection, sepsis, and post-operative infection was 67 percent higher than the non-diabetic group. In addition, the study authors noted a stronger association between diabetes and hospitalization related to infection in younger participants and Black patients … read more
A report of 12 months’ of data collected from a diabetic foot clinic at a public hospital in Phnom Penh, Cambodia
This report interprets data gathered from a diabetic foot ulcer clinic in an outpatient department of a public hospital in Phnom Penh, Cambodia. The data were gathered between September 2019 and August 2020 and were entered into a Microsoft Excel™ spreadsheet. It gives basic demographic information of Cambodian patients with diabetic foot ulceration and provides data that can be used to measure any future research or audit. The data collection timeframe … read more
Medicinal Plants as Efficacious Agents for Diabetic Foot Ulcers: A Systematic Review of Clinical Studies
A diabetic foot ulcer (DFU) is a chronic, nonhealing wound that occurs in approximately 15% to 25% of patients with diabetes, and amputation is necessary in approximately 5% to 24% of these patients. Medicinal plants have demonstrated promising wound healing activities in animal models of DFUs as well as in clinical studies. These plants, which are described as medicinal in different regions of the world, are not considered to be standard medicinal treatments in Western medicine at this time. Some medicinal products, such as bromelain—an herbal protease currently used for enzymatic debridement of wounds—have been obtained from plants, showing the important role of these natural products as sources of wound healing agents. This paper aims to review clinical studies on the effects of medicinal plants in patients with DFUs based on the improvement of local and systemic parameters related to wound healing. Electronic databases including PubMed, Scopus, and Cochrane Library were searched for studies from inception through May 2019 using the keywords “diabetic foot ulcer” … read more
Infection-Related Hospitalizations High for Adults With Diabetes
People with diabetes may face a higher risk for hospitalization for any infection, a new analysis suggested.
In a prospective study of over 12,000 middle-age adults, those with diabetes had a 67% higher risk for infection-related hospitalization compared with adults free of diabetes over the course of nearly 30 years (HR 1.67, 95% CI 1.52-1.83), reported Elizabeth Selvin, PhD, MPH, of Johns Hopkins Bloomberg School of Public Health in Baltimore, and colleagues … read more
Introduction to the work of IWGDF Guidelines
Every 20 seconds somewhere in the world someone loses a leg due to the complications of diabetes. After such amputations, over half of these people will die within 5 years. At this moment, millions of people with diabetes suffer from poorly healing foot ulcers, which usually develop as a result of several factors. Successfully managing these ulcers, or, even better, preventing them, depends on the close collaboration of various types of health professionals; they must integrate up-to-date care in their specialty into an effective multidisciplinary foot team. The key factors for optimal outcomes are that team members share common goals and follow evidence-based, comprehensive guidelines … read more
New research a ‘step change’ for diabetes patients
Millions of people with diabetes are at risk of developing foot ulcers, which often lead to amputations and other health complications. Now, Scientists from the Centre for Biomechanics and Rehabilitation Technologies (CRBT) have developed a new method to reliably detect this risk without the need for complex electronic in-shoe sensors … read more
A Compendium of Perspectives on Diabetes: A Challenge for Sustainable Health in the Modern Era
Diabetes is a chronic illness. Hyperglycemia is the characteristic of this disorder. Diabetes is a global crisis which affects the economy and health of all nations. Over the last decades, the number of individuals living with diabetes has significantly increased worldwide. Asia is a key epicenter of the emerging diabetes epidemic, with China and India the two nations having the highest number of diabetic people. Economic development, modernization, unhealthy diet, population aging, and sedentary lifestyles are the major factors responsible for the increasing diabetes epidemic. Diabetes is associated with several complications, and cardiovascular disease is the most important cause of morbidity and mortality among people with diabetes. These life-threatening problems can be prevented or delayed by proper management of diabetes. Lifestyle modification is an important factor to decrease the diabetes risk. The frequency of diabetic complications will rise if there is a lack of cost-effective and sustainable interventions. Hence, prevention of diabetes and its complications such as diabetic retinopathy and cardiovascular disease … read more
T-Natural Killers and Interferon Gamma/Interleukin 4 in Augmentation of Infection in Foot Ulcer in Type 2 Diabetes
Epidemiology studies have shown that diabetes has the highest incidence of any chronic disease worldwide and is a huge threat to human health. Diabetes is clinically divided into types I and II.1 The prevalence of type II diabetes mellitus (T2DM) increases with age across all regions and income groups.2 Still, the prevalence is increasing in young age groups due to unhealthy life routines present since childhood … Insulin resistance (IR) associates with T2DM. Diabetes-related foot complications are important causes for disability worldwide. More than one-third of patients with diabetes worldwide will develop diabetic foot ulcer (DFU), which can progress to diabetic foot infection (DFI), and gangrene, consuming most of the healthcare costs dedicated for patients with diabetes. Around 17% of DFI will require amputation. Studies showed that patients with diabetes fear amputation more than death. The DFI patients will demand extensive debridement … continue
Predictive model identifies risk factors for major adverse limb events in diabetes
A risk score may be able to identify adults with type 2 diabetes at high risk for major adverse limb events, including in those without a history of peripheral artery disease, according to a study published in Diabetic Medicine … “This post hoc analysis of the EXSCEL trial yielded a predictive score for major adverse limb events among participants with diabetes that had a C statistic of 0.822, generally considered as very good … … continue
Diabetes doubles risk for hospital-acquired foot ulcers
Patients with diabetes have at least double the risk for developing hospital-acquired foot ulcers vs. those without diabetes, according to a study published in BMJ Open Diabetes Research & Care.
In a prospective, multilevel regression analysis, Frances Wensley, PhD, MBBS,formerly of the Royal Free Hospitals NHS Foundation Trust in London, and colleagues analyzed data from 18,946 patients with 28,642 admissions of at least 2 days to the Ipswich Hospital NHS Trust between October 2008 and September 2010, including 3,076 individuals with diabetes with 5,043 admissions. Patients included in the analysis were aged at least 50 years and developed a hospital-acquired foot ulcer at least 48 hours after hospital admission. For all admissions, the analyses included data on diabetes, heel ulcer, length of stay and other covariates. The researchers compared patients with vs. without diabetes … read more
Nutrition Management of Individuals with Diabetes and Pressure Injuries
by Dr. Nancy Munoz, DCN, MHA, RDN, FAND
The presence of diabetes can have a negative impact on wound healing rates. Increased glucose levels can stiffen the arteries and contribute to narrowing of the blood vessels. This can influence pressure injury development and is a risk factor for impaired wound healing.
Overview of Diabetes Mellitus
Diabetes is an illness in which the individual’s blood glucose level is above the established range. Glucose is present in the foods we eat. Most foods contain a blend of carbohydrates, proteins, and fats. The amount of each of these nutrients in the foods we consume determines how quickly the body transforms food into glucose. For instance, consuming carbohydrates affects blood glucose levels one to two hours after the meal. Ingesting protein has very little influence on blood glucose levels, and the glucose from the fat in foods is slowly absorbed and does not contribute to increased glucose levels … read more
Retired surgeon leads local diabetes study
SHERIDAN — After working as an orthopedic surgeon for 20 years, Dr. Scott Nickerson was forced into an early retirement by diabetes.
After graduating from the Johns Hopkins University School of Medicine, Nickerson moved to Sheridan in 1977 to work as an orthopedic surgeon at Sheridan Orthopaedics, which was a small three-doctor practice at the time.
One of the many complications of diabetes is neuropathy, nerve damage that can lead to pain, weakness and loss of sensation in the extremities.
Nickerson said after living with diabetes for about 10 years, he began to notice his hands were getting clumsy.
“I would drop tools a little bit or just not have quite the sensation you would depend on to do the work,” Nickerson said. “Plus it would hurt me a lot to be on my feet.”
Nickerson decided to retire so the effects of his neuropathy would not affect his work as a surgeon … read more
The Whole Patient Approach
Addressing Common Comorbidities That Affect Wound Healing
When developing the plan of care for the patient with a chronic wound, it is imperative first to look at the “whole” patient and not just the “hole” in the patient.1 As we do, we are able to review any medical conditions or disease states that may affect wound repair and healing. Millions of Americans are affected by chronic wounds each year. These wounds include causes such as diabetic foot ulcers, venous leg ulcers, arterial insufficiency, and pressure ulcers. Common comorbid conditions that can affect healing include diabetes, venous insufficiency, peripheral arterial disease, cardiopulmonary and oxygen transport conditions, immune deficiencies, and dementia.2 This discussion is focused on these conditions and factors that contribute to chronic wounds and their management … read more
Diabetes UK commits £2.6 million to new research
- New funding will be split between 14 new research projects and five new PhD grants
- New research includes projects investigating whether medieval remedies can be used to treat foot ulcers, and if sleep disturbances can predict Type 2 diabetes
Diabetes UK has committed to invest £2.6 million in 19 brand new projects which aim to make life-changing improvements in diabetes care, and reduce people’s risk of Type 2 diabetes.
The funding will be given to projects looking into Type 1, Type 2 and gestational diabetes. In one of these projects, Dr Freya Harrison, from the University of Warwick, will be using medieval remedies to find new sources of antibiotics. She has already discovered a combination that can kill antibiotic-resistant bacteria in the lab. Dr Harrison will study this remedy further to investigate how it works and if it could be used to treat infected foot ulcers in the future.
There are more than 20 leg, foot and toe amputations each day due to diabetes, four out of five of which could be prevented. This research hopes to reduce the number of diabetes-related amputations and cases of sepsis, by treating foot ulcer infections more effectively.
Dr Martin Rutter, from the University of Manchester, has also been awarded Diabetes UK funding to find out if sleep problems can help predict who might be at risk of Type 2 diabetes. He will also look at whether sleep patterns in people with Type 2 diabetes can affect their blood glucose control, and their risk of serious diabetes-related complications, such as amputation, heart disease and blindness … read more
Toward Eliminating Diabetic Foot Amputation In The Next Generation

David G. Armstrong, professor of surgery at the Keck School of Medicine of USC
Humanity crossed a line in 2009: For the first time in history, more people in the last decade died from non-communicable disease than from all the plagues in the world combined. We’ve entered what science pundit Steve Jones has, in a rather macabre but perceptive manner, dubbed the Age of Decay.
First was the Age of Disaster — 95 percent of human history — when people died from starvation, accidents, violence and cold temperatures. Around 12,000 years ago, we learned to “circle the wagons,” if you will, as a species. As we became agrarian, we moved closer together to store food. A natural byproduct of this was the Age of Disease, when plagues decimated populations. We’re now in the Age of Decay, when the big killers are non-communicable diseases — cancer, cardiovascular disease and diabetes. Pulmonary disease is fourth.
The longer that I have labored in my line of work, the more I realize it is the height of hubris as a clinician to think that I can “fix” anyone. Rather, I think the best thing I can do is help folks move through the world a little bit better. Our goal in this age as clinicians, scientists, policymakers, is to think not about fixing everything but rather to delay decay.
We all rightly take cancer and heart attacks seriously. Diabetes, however, has not risen to that level. If one were an evil deity and wanted to sock it to humanity, one wouldn’t pick something like cancer or a heart attack. Those are often far too dramatic. One would rather choose diabetes: It is silent, sinister and it happens in the background. No one sees it coming. How, then, does diabetes cause amputations?
Assessment and management of foot ulcers
for people with diabetes.
Major Recommendations
The levels of evidence supporting the recommendations (Ia, Ib, IIa, IIb, III, IV) are defined at the end of the “Major Recommendations” field.
Practice Recommendations
Assessment
Recommendation 1.0
Obtain a comprehensive health history and perform physical examination of affected limb(s).
(Level of Evidence = Ib–IV)
Recommendation 1.1
Identify the location and classification of foot ulcer(s) and measure length, width, and depth of woundbed.
DIABETIC FOOT: FACTS AND FIGURES
The management of diabetic foot: A clinical practice guideline by the Society ….
A clinical practice guideline by the Society for Vascular Surgery in collaboration with the American Podiatric Medical Association and the Society for Vascular Medicine
Diabetes is one of the leading causes of chronic disease and limb loss worldwide, currently affecting 382 million people. It is predicted that by 2035, the number of reported diabetes cases will soar to 592 million.1 This disease affects the developing countries disproportionately as >80% of diabetes deaths occur in low- and middle-income countries. As the number of people with diabetes is increasing globally, its consequences are worsening. The World Health Organization projects that diabetes will be the seventh leading cause of death in 2030.3 A further effect of the explosive growth in diabetes worldwide is that it has become one of the leading causes of limb loss. Every year, >1 million people with diabetes suffer limb loss as a result of diabetes. This means that every 20 seconds, an amputation occurs in the world as an outcome of this debilitating disease. Diabetic foot disease is common, and its incidence will only increase as the population ages and the obesity epidemic continues … read more
Diabetic Wound Healing and LED Irradiation
Introduction: Light-Emitting Diode Therapy for Chronic Non-Healing Diabetic Wounds
Diabetes mellitus is frequently associated with chronic non-healing wounds, many of which result in amputation. The combination of peripheral vascular disease, neuropathy, and impaired immune function contributes to a higher risk of injury and deficiency in healing. Wound healing is a complex process comprising eight important factors: (1) collagen synthesis, (2) cell migration, (3) cell cycle and differentiation, (4) angiogenesis and growth hormone, (5) blood clotting, (6) extracellular matrix and focal adhesion, (7) calcium ion signaling, and (8) immune and inflammatory response. In the diabetic cell, all these processes malfunction, with the exception of collagen synthesis, cell migration, and cell cycle or differentiation.
Previous studies found an association between diabetes and the precursor protein pro-opiomelanocortin (POMC) gene. POMC is normally expressed in pituitary melanotroph and corticotroph cells and functions to control body weight. Studies have suggested that a mutation in the POMC gene leads to early-onset type 2 diabetes and obesity. This correlation is under investigation for its potential use in diabetic therapy.
Light-emitting diode (LED) phototherapy at 660 and 890nm has been shown to significantly accelerate wound healing in normal, healthy patients. This therapy works through molecules with porphyrin structures that are able to trap photon energy and subsequently activate downstream processes. The current study investigated the results of a range of different LED phototherapies on gene expression and cellular function of diabetic cells compared with normal, healthy cells … read more
Living with a Diabetic Foot Ulcer
Patient Perspective:
An Interview with Robert S. Meyer by Janet L. Kuhnke Robert Meyer lives with diabetes and a foot ulcer. He has attended multiple Wounds Canada events as both a speaker and to learn more about how he can manage his condition, heal his wound and prevent further foot complications. He is interviewed here by wound care clinician and educator Janet Kuhnke.
Janet L. Kuhnke: Robert, you attended the fall 2017 Wounds Canada conference in Mississauga, Ontario. Can you tell me what this was like for you as a patient?
Robert S. Meyer: I was there as a patient and a speaker, but it was not until I got back home that the depth of my message sank in. First, I wanted to do my talk as a tribute to my mother, who had a nasty death due to the complications of diabetes. Second, if my message could help someone, it would be worth it all. Not just for other patients but for other service providers who need to find their own inner voice and become advocates for themselves or others, no matter the issue. Third, telling my story has a profound impact on my own healing journey. Now I know why victims of trauma need to tell their story as part of their healing. The important part is knowing that someone has listened and heard … read more
Diabetic foot ulcers heal faster with probiotic supplementation
Findings from a randomized controlled trial revealed that patients with a diabetic foot ulcer, who received probiotic supplementation for 12 weeks, experienced faster wound healing coupled with an improved glycemic and lipid profile compared with patients assigned a placebo … read more.
Research reveals the true impact of diabetic foot ulcers
The prognosis for people with an infected diabetic foot ulcer is worse than was previously thought, according to new research.
More than half the patients in the research study did not see their ulcer heal over a year – and one in seven had to have part or all of their foot amputated.
Foot ulcers are open wounds and they affect around a quarter of the 3.3 million people in the UK living with diabetes.
The wounds develop because diabetes damages the nerves and blood vessels in the feet.
These wounds are chronic, slow to heal and prone to infection, and it is infection that normally leads to some of the severe consequences such as losing a limb or multiple amputations.
The research, led by Professor Andrea Nelson at the University of Leeds, set out to examine the outcomes for people with infected diabetic foot ulcers and the results underline the need for people at risk of foot ulcers to be closely monitored.