Tag: Chronic Wounds


Study of 236 patients reveals utility of MolecuLight i:X® in detection and management of wound-related cellulitis
Published results describe use of point-of-care imaging for the early detection and proactive management of wound-related cellulitis
TORONTO, Oct. 12, 2021 /PRNewswire/ – MolecuLight Inc., the leader in point-of-care fluorescence imaging for real-time detection of wounds containing elevated bacterial loads, announced the publication in International Wound Journal1 of an independent prospective observational study examining the impact of incorporating fluorescence imaging into standard care for the diagnosis and management of wound-related cellulitis. Dr. Charles Andersen, a surgeon at the Madigan Army Medical Center, led this study on wound-related cellulitis, defined as an invasion of bacteria from chronic wounds into the adjacent dermis.
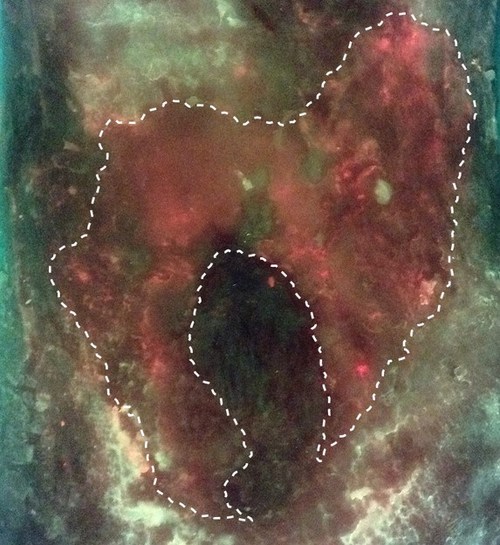
The publication, “Diagnosis and Treatment of the Invasive Extension of Bacteria (Cellulitis) from Chronic Wounds Utilizing Point-of-Care Fluorescence Imaging“, included 236 patients visiting Madigan’s outpatient wound care center over a 16-month period between January 2020 and April 2021. In the study, wound-related cellulitis was diagnosed in 6.4% (15/236) of patients. Consistent among all patients diagnosed with wound-related cellulitis was an irregular pattern of red (bacterial) fluorescence visualized on the MolecuLight i:X point-of-care imaging system that extended beyond the wound bed and periwound. This unique pattern of red fluorescence could not be removed through cleansing or debridement.
Cellulitis is a serious clinical condition, accounting for 10% of all infectious disease-related US hospitalizations2 and up to $3.7 billion in costs annually 3. Cellulitis can lead to serious complications including bacteremia, necrotizing fasciitis, endocarditis, or shock4,3. Severe cellulitis in patients with other comorbid conditions may result in death. Timely and accurate diagnosis of cellulitis is notoriously challenging due to a lack of gold standard diagnostic techniques and a similar clinical presentation as other inflammatory conditions (e.g., stasis dermatitis). In those patients misdiagnosed, 85% experience avoidable hospital admission and 92% receive unnecessary antibiotics5.
“The results of this study show how MolecuLight point-of-care imaging presents an intriguing solution to revealing extension of bacteria into tissue, reducing misdiagnosis of wound-associated cellulitis, and enabling more proactive early treatment, particularly in patients lacking obvious symptoms”, says Dr. Charles A. Andersen, Chief, Vascular/ Endovascular and Limb Preservation Surgery Service (Emeritus), Chief Wound Care Service and Medical Director Wound Care Clinic at Madigan Army Medical Center, Tacoma, WA. “Given that at least 30% of cellulitis cases are misdiagnosed,6,5 the addition of consistent and objective information provided by fluorescence scans can significantly reduce the uncertainty associated with diagnosis of wound-related cellulitis. In addition, the use of fluorescence imaging to support earlier detection and proactive management of wound-related cellulitis can limit progression of infection and avoid the need for intravenous antibiotics and the high costs associated with inpatient admission”.
An example case of wound-related cellulitis from the study is shown (above) where the wound does not appear to have cellulitis or elevated bacterial burden upon assessment with standard-of-care clinical signs and symptoms (left). In contrast, when imaged with the MolecuLight i:X (right), an irregular pattern of red (bacterial) fluorescence extending beyond the wound bed and periwound is visible, and could not be removed with vigorous cleansing, indicating that the bacteria are located subsurface. This pattern of red fluorescence, demonstrating invasive extension of bacteria into surrounding tissues, was consistent in all wounds in the study where wound-related cellulitis was diagnosed.
Dr. Andersen will present the findings of this publication in a talk titled, “Diagnosis and Treatment of the Invasive Extension of Bacteria (Cellulitis) from Chronic Wounds Utilizing Point-of-Care Fluorescence Imaging“ at the upcoming clinical conference, SAWC (Symposium on Advanced Wound Care) Fall 2021 on Sunday, October 31, 2021 at 9:00 am at Caesars Palace in Las Vegas, Nevada.
|
References |
|
|
1 |
Andersen, C.A. et al, “Diagnosis and Treatment of the Invasive Extension of Bacteria (Cellulitis) from Chronic Wounds Utilizing Point-of-Care Fluorescence Imaging“, International Wound Journal 2021: 1-13 |
|
2 |
Lazzarini L et al, J Infect. 2005;51(5):383-389. |
|
3 |
Raff AB et al, JAMA. 2016;316(3): 325-337. |
|
4 |
Pasternack MS. Mandell, Douglas, & Bennett’s Principles & Practice of Infectious Diseases. Vol 1; Phil., PA: Churchill Livingstone/Elsevier; 2010:1289-1312. |
|
5 |
Weng QY et al, JAMA Dermatol. 2017;153(2):141-146. |
|
6 |
Levell NJ et al, Br J Dermatol. 2011;164(6):1326-1328. |
About MolecuLight Inc.
MolecuLight Inc., a privately-owned medical imaging company that has developed and is commercializing its proprietary fluorescent imaging platform technology in multiple clinical markets. MolecuLight’s first commercially released device, the MolecuLight i:X fluorescence imaging system and its accessories provide a point-of-care handheld imaging device for the global wound care market for the detection of wounds containing elevated bacterial burden (when used with clinical signs and symptoms) and for digital wound measurement. The company is also commercializing its unique fluorescence imaging platform technology for other markets with globally relevant, unmet needs including food safety, consumer cosmetics and other key industrial markets.
Image:
Download at: https://moleculight.box.com/s/oab22c1vi8ud1j8oymylbfogp2lg12bk
SOURCE MolecuLight
Related Links
Researchers explore promising treatment for MRSA ‘superbug’
A new Cornell study has found the antimicrobial properties of certain stem cell proteins could offer a potential treatment to reduce infection in skin wounds.
Treating wounds with the secretion of a type of stem cell effectively reduced the viability of methicillin-resistant Staphylococcus aureus – better known as MRSA – according to a new study from researchers at the Baker Institute for Animal Health, part of the College of Veterinary Medicine (CVM). Moreover, the secretion stimulated the surrounding skin cells to build up a defense against the bacterial invader, the researchers found … read more
Microneedle patch penetrates biofilms to treat chronic wounds
Chronic wounds such as diabetic foot ulcers can be very difficult to treat, partially because of antibiotic-resistant “biofilms” that form over the affected tissue. A new type of microneedle patch, however, has been shown to deliver medication through such films … Bacterial bioflms are made up of colonies of bacteria that stick together by building up a slimy polymer matrix. Unfortunately, topically applied antibiotics and other medications have difficulty penetrating that matrix, so they can’t reach the infected tissue underneath … read more
Antibacterial nanozymes: Healing chronic wounds with nanochemistry
Chronic infected wounds are often highly problematic for diabetic patients. However, a team of Chinese researchers has now developed a targeted approach to wound healing that makes use of nanomedicine, and their research has been published in the journal Angewandte Chemie. The researchers were able to deactivate wound-infecting bacteria using a solution of nanocapsules that alter the wound environment and unleash reactive oxygen species … read more
Screening for Depression in Patients with Chronic Wounds
Wounds with a duration longer than 30 days are considered chronic. For example, diabetic foot ulcers comprise a large majority of these wounds and often exceed the expected 12-week healing period because of underlying factors that cannot be fully corrected.1 Patients with chronic wounds face considerable psychological stress because they need continuous medical care and frequent visits to healthcare facilities. The presence of these wounds significantly disrupts the daily life of patients, including changes in sleeping patterns, diet, and mobility. Loss of mobility may lead to feelings of loneliness, powerlessness, and dependency, as patients rely on family or friends to help fulfill their basic needs such as commuting, activities of daily living, and personal hygiene. Further, patients may experience chronic pain, exudate, and odor, which negatively impact social interactions, relationships, sexuality, and self-confidence. All of these psychosocial factors add up and may lead to a slow onset of anxiety and depression in patients with chronic wounds … read more
Improved wound management at lower cost: a sensible goal for Australia
Chronic wounds cost the Australian health system at least US$2·85 billion per year. Wound care services in Australia involve a complex mix of treatment options, health care sectors and funding mechanisms. It is clear that implementation of evidence‐based wound care coincides with large health improvements and cost savings, yet the majority of Australians with chronic wounds do not receive evidence‐based treatment. High initial treatment costs, inadequate reimbursement, poor financial incentives to invest in optimal care and limitations in clinical skills are major barriers to the adoption of evidence‐based wound care. Enhanced education and appropriate financial incentives in primary care will improve uptake of evidence‐based practice. Secondary‐level wound specialty clinics to fill referral gaps in the community, boosted by appropriate credentialing, will improve access to specialist care. In order to secure funding for better services in a competitive environment, evidence of cost‐effectiveness is required. Future effort to generate evidence on the cost‐effectiveness of wound management interventions should provide evidence that decision makers find easy to interpret. If this happens, and it will require a large effort of health services … read more
Smart plaster could accelerate the healing of chronic wounds
Circulatory disorders, diabetes or lying in the same position for extended periods can all lead to chronic wounds that do not heal. There are hardly any effective treatment options. A materials science research team from Kiel University (CAU), together with colleagues from the University Medical Center Schleswig-Holstein (UKSH), Harvard Medical School, U.S., and Dankook University in South Korea, has developed a wound patch with enhanced healing functions which can be individually adapted for each patient. The 3D-printed patch has antibacterial properties, supplies the wound with oxygen and moisture, and supports the formation of new tissue … read more
A molecular approach to maggot debridement therapy with Lucilia sericata and its excretions/secretions in wound healing
Chronic wounds caused by underlying physiological causes such as diabetic wounds, pressure ulcers, venous leg ulcers and infected wounds affect a significant portion of the population. In order to treat chronic wounds, a strong debridement, removal of necrotic tissue, elimination of infection and stimulation of granulation tissue are required. Maggot debridement therapy (MDT), which is an alternative treatment method based on history, has been used quite widely. MDT is an efficient, simple, cost-effective and reliable biosurgery method using mostly larvae of Lucilia sericata fly species. Larvae can both physically remove necrotic tissue from the wound site and stimulate wound healing by activating molecular processes in the wound area through the enzymes they secrete. The larvae can stimulate wound healing by activating molecular processes in the wound area through enzymes in their excretions/secretions (ES). Studies have shown that ES has antibacterial, antifungal, anti-inflammatory, angiogenic, proliferative, hemostatic and tissue-regenerating effects both in vivo and in vitro. It is suggested that these effects stimulate wound healing and accelerate wound healing … read more
Older Adults More Likely to Develop Chronic Wounds, Research Shows
Older adults are at a higher risk of developing chronic wounds due to complications associated with aging, research published in the Journal of the American Geriatrics Society showed.
Chronic wounds can be defined as wounds that fail to re-establish anatomic and functional skin integrity over 1–3 months through a timely reparative process. Overlapping descriptions and different wound categories makes understanding the prevalence of chronic wounds difficult, but data published in 2017 revealed that chronic wounds affect 5.7 million Americans and incur annual costs of $20 billion … read more
Inexpensive collagen-based dressing could help heal chronic wounds
Currently, many chronic wound dressings incorporate harvested natural biological tissue. Obtaining those tissues from donors – and working them into the material – is typically a very complex process. According to Michigan State University (MSU), this means that such dressings may ultimately cost up to US$1,000 each … Seeking a more affordable alternative, an international team led by MSU’s Asst. Prof. Morteza Mahmoudi has instead looked to collagen, which is the main structural protein in the extracellular matrix of the body’s connective tissues … read more
Kent Imaging Inc. Receives Health Canada Approval on SnapshotNIR v3.0
Kent Imaging has announced Health Canada’s approval for SnapshotNIR V3.0 (KD204) – now available for shipping in both official languages. This upgrade provides significant feature enhancements to the imaging technology that advances tissue assessment in acute and chronic wounds. The multitude of features include the ability to image most skin tones (overcoming the melanin barrier), linear and surface area wound measurements, easy report generation with image comparisons, and enhanced patient file management, to name a few.
“As a firmly Canadian company, we are excited to release this enhanced version of SnapshotNIR into the country. This is another critical step in our goal of delivering effective wound care and surgical solutions to care providers and improving patient outcomes,” says Pierre Lemire, Kent’s CEO. “The updates to SnapshotNIR V3.0 will make it easier and faster than ever to bring critical real-time and point-of-care data to the treatment path.”
SnapshotNIR utilizes near-infrared light to determine tissue oxygen saturation (StO2), which is a key indicator of tissue health. Ideal for microcirculation assessment, it conveys a comprehensive picture of the healing capacity of wounds or surgical tissue. This critical information is used to support clinical judgment in choosing, evaluating, and tracking treatment and surgical options throughout the care continuum … read more
High Levels of Oxidative Stress and Skin Microbiome are Critical for Initiation and Development of Chronic Wounds in Diabetic Mice
A balanced redox state is critical for proper healing. Although human chronic wounds are characterized by high levels of oxidative stress (OS), whether OS levels are critical for chronic wound development is not known. For these studies, we used our chronic wound model in diabetic mice that has similar characteristics as human chronic wounds, including naturally developed biofilm. We hypothesize that OS levels in wound tissues are critical for chronic wound initiation and development. We show that increased OS levels in the wound correlate with increased chronicity. Moreover, without increased OS levels, biofilm taken from chronic wounds and placed in new excision wounds do not create chronic wounds. Similarly, high OS levels in the wound tissue in the absence of the skin microbiome do not lead to chronic wounds. These findings show that both high OS levels and bacteria are needed for chronic wound initiation and development … read more
Bromelain-based enzymatic debridement of chronic wounds: Results of a multicentre randomized controlled trial
Chronic wounds are estimated to affect over 6 million people annually in the United States with an estimated annual cost of $25 billion. Debridement represents a key step in their management and is considered a basic necessity to induce the functional process of tissue repair. However, there is an unmet need for an efficient rapid acting non-surgical debridement agent. Bromelain-based enzymatic debridement has been proven to provide an effective, selective and safe non-surgical debridement in deep burns. EscharEx (MediWound Ltd, Yavne, Israel), is a bromelain-based enzymatic debridement agent currently in development for chronic wounds. The aim of this study was to assess its safety and efficacy in chronic wounds. Seventy-three patients suffering from a lower extremity ulcer of diabetic/venous insufficiency/post-surgical/traumatic aetiology were enrolled in a multicentre … read more
When Should I Perform Point-of-Care Fluorescence Imaging of Wound Bioburden? Guidelines Based on Delphi Consensus
Bacteria and biofilm plague chronic wounds, impair the healing process, and can increase the risk of infection and antibiotic overprescribing. Fluorescence imaging of bacterial burden (MolecuLight i:X) is the only point-of-care solution to visualize the presence of significant bacterial burden in wounds. This information, when added to standard of care, supports informed clinical decision making and more proactive bacterial management practices. This point-of-care imaging technology is quickly becoming a standard in wound care … View webinar start time in your timezone.
When Should I Perform Point-of-Care Fluorescence Imaging of Wound Bioburden? (webinar)
Bacteria and biofilm plague chronic wounds, impair the healing process, and can increase the risk of infection and antibiotic overprescribing. Fluorescence imaging of bacterial burden (MolecuLight i:X) is the only point-of-care solution to visualize the presence of significant bacterial burden in wounds. This information, when added to standard of care, supports informed clinical decision making and more proactive bacterial management practices. This point-of-care imaging technology is quickly becoming a standard in wound care … View webinar start time in your timezone
Refractory Wounds: Systemic Factors Affecting Repair – Extrinsic Factors (Part 2 of 4)
Refractory wounds are a significant worldwide health problem, affecting 5 to 7 million people per year in the United States alone, as discussed in a prior blog. Wounds that fail to heal not only impact quality of life, but also impose a significant physical, psychosocial, and financial burden. Additionally, individuals with refractory wounds often experience significant morbidity and sometimes mortality. Wound infections and amputations are common in this population, and chronic conditions often exist as well … read more
Refractory Wounds: Etiologic Factors and Management (a Four-Part Series)
Refractory wounds comprise a significant worldwide health problem, affecting 5 to 7 million people per year in the United States alone. Wounds that fail to heal not only impact quality of life but also impose a significant physical, psychosocial, and financial burden. Additionally, individuals with refractory wounds often experience significant morbidity and sometimes mortality. Wound infections and amputations are common in this population, and chronic conditions often exist as well … read more
Clinical Evidence Outlines the Need for Early Advanced Standard of Care with Real-world Chronic Wound Case Reviews
Principle Investigators, Dr. Pons and Dr. Teichman, discuss a Pooled analysis of 434 wounds at 30 centers that supports the use of PuraPly AM to advance wounds out of the inflammatory phase. Discussions include presentations of real-world case reviews … Click HERE to view.
Decreasing Pain and Increasing the Rate of Chronic Wound Closure With the Use of a Noninvasive Bioelectronic Medical Device: A Case Series
Chronic wounds are a source of significant morbidity. Medical and scientific efforts are ongoing to further therapeutic modalities improving pain scores and augmenting healing while decreasing complications and reducing the social and economic burden of wounds. Electrical current therapy, or electrical stimulation (ES), has been shown to decrease and modulate both acute and chronic pain; however, understanding of the role of ES in wound closure is limited. Objective. This single-center case series reports use of a topical ultrahigh frequency ES (UHF-ES) therapy to decrease wound pain and improve the rate of closure in difficult-to-heal wounds in 9 patients. Materials and Methods. Initially, each patient underwent individualized care of their chronic wounds for a minimum of 8 weeks … read more
Advanced Oxygen Therapy Inc. Named Among the 10 Most Innovative MedTech Solution Providers to Watch in 2021
(https://thehealthcareinsights.com/advanced-oxygen--inc-dedicated-to-resolving-acute-and-chronic-wounds-through-its-unique-multi-modality-two2therapy/) how AOTI is dedicated to resolving acute and chronic wounds through its patented cyclical-pressure Topical Wound Oxygen (TWO2) therapy. Thereby providing clinically proven complete healing outcomes and wound protective care to high-risk patients safely at home. Maintaining such continuity-of-care has become even more vital during the recent COVID-19 pandemic read more
A flexible multiplexed immunosensor for point-of-care in situ wound monitoring
Chronic wounds arise from interruption of normal healing due to many potential pathophysiological factors. Monitoring these multivariate factors can provide personalized diagnostic information for wound management, but current sensing technologies use complex laboratory tests or track a limited number of wound parameters. We report a flexible biosensing platform for multiplexed profiling of the wound microenvironment, inflammation, and infection state at the point of care. This platform integrates a sensor array for measuring inflammatory mediators [tumor necrosis factor read more
Keys To Addressing Forefoot Plantar Ulcerations
The Centers for Disease Control and Prevention (CDC) estimates one in ten Americans have diabetes and one in three have prediabetes … Diabetes is also increasing among younger populations and can lead to sleep apnea, cardiovascular disease, pulmonary disease and risk of cancer … One major complication of diabetes is diabetic peripheral neuropathy (DPN), seen in 50 percent of the geriatric population with diabetes … continue
Car crashes and chronic wounds
The health epidemic no one is talking about
Chronic wounds impact the lives of millions of Americans, yet the stories of those suffering are rarely told. As a result, chronic wounds have turned into a silent epidemic that remains largely invisible to the general public. Twenty-five years ago, Kevin Fontenot was one of those people, living his life generally unaware of this horrible condition, which is often caused by other diseases such as renal failure, diabetes, circulatory problems or malnutrition. That is, until he himself fell victim to it … read more
Oxygen therapies for wound healing: EWMA findings and recommendations
For wounds to heal, it is essential that macro- and microcirculation is restored in the surrounding tissue (Niinikoski et al, 1991; Gottrup, 2004a). One of the most urgent requirements is oxygen, as it is critically important for the reconstruction of new vessels and connective tissue, and also enables resistance to infection … View PDF
Wound Care Patient Outcomes: Establishing Trust to
Improve Wound Healing Results
Last spring, I encountered that specific type of patient we sometimes meet, the one who has been through the chronic wound care revolving door so many times that he or she sets out on his or her own path and refuses any byways diverting from it.
Ms. A had stage 3 lymphedema after a left knee replacement opened the hidden trap door of undiagnosed lymphedema several years before her admission to our inpatient rehab facility. Her reason for admission was debility from urinary tract infection (UTI). Comorbidities of obesity, severe arthritis of the right knee, diabetes, and chronic lymphedema wounds on both legs were exacerbating factors making discharge home difficult from the acute hospital … read more
Material could offer ‘smarter’ wound healing
A new study takes a step toward the development of smarter skin grafts that facilitate healing while minimizing infection for chronic skin wounds.
“Our group has expertise in developing new polymers and functional surface assemblies for biomedical applications,” says Svetlana Sukhishvili, professor and director of the soft matter facility at Texas A&M University.
“At Texas A&M we investigated how to build a stimuli-responsive polymeric material that could absorb and release antibiotics when prompted by a physiologically relevant stimuli,” explains lead researcher Victoria Albright, a graduate student materials science and engineering department … read more
SomaGenics Awarded Multi-Year Funding for Hepatitis Delta Virus Therapeutic Program
SANTA CRUZ, Calif., July 30, 2018 /PRNewswire/ — SomaGenics, Inc. announces the award of a three-year, $2.9 million NIH grant in support of its Hepatitis Delta Virus (HDV) therapeutic program under Principal Investigator and SomaGenics CEO Brian H. Johnston, Ph.D. This Phase II grant, from the NIH’s Small Business Innovation Research (SBIR) program, continues the development of SomaGenics’ novel RNA interference (RNAi)-based approach under a Phase I SBIR grant and will fund late-stage preclinical studies and preparations for clinical trials.
HDV infection, which requires concurrent or prior infection with the hepatitis B virus, results in the most severe form of viral hepatitis, and no HDV-specific therapy exists. Chronic HDV has a 20% mortality rate and its incidence is rising globally. The establishment of U.S.–based Hepatitis Delta Connect (hepconnect.org), a public outreach program, highlights recent efforts to increase patient and physician awareness about the pressing need for HDV screening and treatment.
SomaGenics’ HDV therapeutic is a novel treatment modality simultaneously targeting the virus at multiple stages of its life cycle using the Company’s proprietary synthetic short hairpin RNA (sshRNA®) technology. “Current clinical treatments suffer from multiple problems including limited efficacy, high relapse rate and toxicity,” according to Anne Dallas, Ph.D., Principal Scientist.
To date, the Company has demonstrated efficacy of its sshRNA® HDV therapeutic in cell culture models and will use the new NIH funding to support efficacy studies in animal models as well as to optimize the Company’s novel delivery platform. “Our combination, multi-target approach reduces the likelihood of treatment resistance and targets non-host entities, lowering the chance of toxicity. We are excited that SomaGenics’ therapeutic may have the potential to cure HDV patients,” explains Dr. Dallas.
Somagenics’ sshRNAs® are highly potent RNAi triggers, with IC50’s in the low picomolar range. sshRNAs® have distinct advantages over the more familiar siRNAs, including the fact that they consist of single chemical entities, simplifying their production and purification, and their lack of off-target effects from “passenger” strand retention. sshRNAs® are suitable for use in many indications in addition to HDV, with therapeutics currently in development for chronic wound healing including diabetic foot ulcers.
SomaGenics, Inc. is a privately held company with offices and laboratories located in Santa Cruz, California. The Company specializes in developing novel RNA-centered approaches to address unmet life science research and medical needs. Core competencies include RNA molecules as therapeutic agents, drug targets and biomarkers as well as the development of innovative kits for RNA analysis.
For information on SomaGenics’ HDV program or the sshRNA® platform, please contact Anne Scholz, VP Business Development, 831-426-7700 x20, 199087@email4pr.com
SOURCE SomaGenics, Inc.
Controlling Bacterial Burden in Chronic Wounds
Bioburden in chronic wounds can be a principal contributor to inflammation, clinical wound infection, and further delayed wound healing. Clinically diagnosing infection in chronic wounds can be problematic because most individuals susceptible to developing chronic wounds are subject to physiological states that often blunt typical infectious responses in various ways.1 These responses include pain, erythema, febrile state, leukocytosis, edema and increased wound exudate, wound odor, etc. For example, a patient with a neuropathic ulcer and diabetes mellitus may not report pain or fever or present with leukocytosis but will have increased edema and wound exudate. A patient with an ischemic ulcer of peripheral arterial disease may report pain, erythema, fever, and leukocytosis but not have perfusion sufficient to produce edema or increased wound exudate.1 It is imperative to understand how to concurrently manage factors that can contribute to infection, as well as assess for symptoms and implement interventions to prevent infection … read more
Smart Bandages Give Better Treatment to Chronic Wounds
Engineers from Tufts University have developed a new prototype bandage that actively monitors the condition of chronic wounds and delivers the appropriate drug treatments to improve the chances of healing.
Chronic skin wounds from burns, diabetes and other medical conditions can overwhelm the regenerative capabilities of the skin and can lead to persistent infections and amputations.
However, the researchers designed the bandages with healing elements and thermoresposive drug carries that deliver tailored treatments in response to embedded pH, and temperature sensors that track infection and inflammation … read more

A smart bandage placed on an arm. Temperature and pH sensors in the bandage (right) are read by a microprocessor (left), which may trigger release of drug from the bandage by sending a current through heating elements. Credit: Tufts University
Restoring the Wound Base: The Role of Tissue Management
Successful utilization of the TIME model for wound bed preparation requires a working knowledge of chronic wound tissue types. In addition, building on this foundational knowledge is the development of accurate wound assessment skills. These components combined will assist the clinician in implementing the appropriate interventions for each wound.
Viable Chronic Wound Tissue Types
The term “viable” describes vascular tissue with dynamic biological activity.
Epithelium: This should be dry to touch and can appear white or light pink; it is composed of restratified keratinocytes arising from the basement membrane of the dermis.
Granulation: This appears light pink to red and should be moist with a bumpy texture. Capillaries give granulation tissue its characteristic color, and collagen made from fibroblasts provides structural support. If granulation tissue is pale (poor perfusion), dark red or ruddy (vascular congestion or stasis), or “bubbly” or friable (bleeds with very gentle contact), it is technically considered non-viable because it will not support migrating epithelial cells … read more
Molecular Diagnosis of SSTIs May Yield Better Clinical Outcomes
Molecular diagnostics such as polymerase chain reaction (PCR)–based tests provide faster, more complete results than traditional culture-based tests, and their use may improve outcomes for patients with chronic wounds and skin and soft tissue infections (SSTIs), according to new findings presented at the 21st Annual MAD-ID Meeting held May 9 to 12 in Orlando, Florida.
About 6.5 million individuals were afflicted with chronic wounds and SSTIs in the United States in 2009.1 The costs of treating associated complications reached upward of $25 billion at that time. A more recent study estimated that annual Medicare spending for all wound types ranged from $28.1 billion to a whopping $96.8 billion in 2014.2
“These costs could potentially be mitigated with the use of rapid diagnostics that have the capability to better identify wound pathogens and thus allow clinicians to provide better clinical care through targeted antimicrobial therapy,” said Tanya Moreno, PhD, vice president of research and development at Millennium Health, citing a Mayo Clinic Proceedings article on the hospitalists’ view of treating SSTIs … read more
Wound Care Clinical Trials: Setting the Record Straight
A recent article by Kaiser Health News misquoted me as saying that we enroll only “healthy” patients in our clinical trials. At moments like this, one feels that something has been overlooked. One of my research coordinators, recalling the serious adverse events (SAEs) of the previous week said, “The only patients sicker than ours are underground.”
Anyone who has ever spent more than ten minutes in a wound clinic knows that our patients are anything but healthy. Our acuity levels mirror the dialysis and transplant units. We check the obituaries when our patients miss appointments.
The Chronic Wound Epidemic
Although it should be, this is not just a minor annoyance. A procession of anecdotal observations on the failing health of the wound care space—in a time of flux and disarray—is neither enlightening nor supportive. The article itself focuses on the use of expensive products in wound care. In comparison to other medical specialties, such as oncology or cardiology, our products are inexpensive and cost effective. Chronic wounds are an unacknowledged epidemic. The huge increase in spending has less to do with the cost of wound care products than it does to the staggering number of patients who need them. Why is wound care research so poorly funded? The National Institutes of Health (NIH) does not even have a wound care division … read more
Treatment of Diabetic Foot Ulcers
Diabetic wound is the most common cause of non-traumatic
lower extremity amputation, and response to traditional
interventions is poor in many patients. The lifetime risk of
developing an ulcer among diabetics is 25%, and recurrent
wounds are common after healing. Stigmatization, social
isolation, unemployment, and depression are some of the
negative consequence of Diabetic Foot Ulcer (DFU) on the
quality of life of diabetics. DFU adds a substantial economic
burden to afflicted patients and health systems, primarily
attributable to frequent hospitalization, medication, surgical
procedures, amputation, prosthesis, rehabilitation, and loss of
productivity … read more
These Plasma Patches Could Replace Antibiotics to Treat Chronic Wounds
The German company Coldplasmatech is using the weirdest state of matter to fight superbugs and accelerate healing.
Star Trek is often credited with inspiring real-life technologies, from wireless gadgets to video conferences. Now, a German company called Coldplasmatech has pioneered a “PlasmaPatch” which, much like Star Trek’s “dermal regenerator,” is designed to disinfect and heal wounds.
The device leverages the properties of plasma, the least familiar state of matter to humans, which is normally found in high-energy environments such as stars. Plasma can also be artificially generated at lower temperatures by applying electrical currents to a gas or liquid insulator … read more
Healogics Shines a Light on Chronic Wounds with Fifth Annual Wound Care Awareness Week
JACKSONVILLE, Fla.–(BUSINESS WIRE)–Healogics, Inc., the nation’s leading provider of advanced wound care services, is proud to sponsor the fifth annual Wound Care Awareness Week from June 4 to June 8, 2018. Throughout this week, Healogics team members from around the country will be working together to shed light on the chronic wound epidemic and bring awareness to the advanced wound care options available. Unfortunately, the incidence of chronic wounds is only expected to rise over the next decade, making awareness and advanced wound care more important now than ever before.
Chronic wounds affect approximately 6.7 million people in the U.S. and an excess of $50 billion is spent annually on treatment. The prevalence of chronic wounds is growing in tandem with an aging population and increasing rates of diseases such as diabetes and peripheral arterial disease, and conditions like obesity and the late effects of radiation therapy. Untreated, chronic wounds can lead to diminished quality of life and possibly amputation of the affected limb. It is in this context that Healogics also created the Wound Science Initiative – a collaborative effort to educate and engage key stakeholders in government and across the healthcare system on the poorly understood and underserved needs of people with non-healing wounds.
About Healogics
Headquartered in Jacksonville, Fla., Healogics and its affiliated companies manage a network of 700 outpatient Wound Care Centers® across the United States and multiple locations in the United Kingdom. Healogics currently has more than 3,000 employees, including nearly 300 employed providers (Healogics Specialty Providers). In addition to the company’s network of outpatient Wound Care Centers, Healogics providers partner with over 400 skilled nursing facilities to care for patients with chronic wounds. More than 300,000 patients were treated by Healogics providers in 2017. For additional information, please visit Healogics.com.
Contacts
Healogics, Inc.
Leslie Niblock, 904-524-2695
Director, Corporate Communications
Leslie.Niblock@healogics.com
Chronic Wound Management
Optimizing the Wound Healing Environment
Chronic wounds are any types of wounds that have failed to heal in 90 days. Identifying the cause of a chronic wound is most important in the healing process. We as clinicians must help bolster advanced wound care by sharing advances in education in evidence-based treatment, prevention, and wound assessment.
A wound must go through hemostasis, inflammation, proliferation, and remodeling, along with various cellular contributions. The scaffolding of the extracellular matrix is what provides the elasticity and tensile strength to the skin structure. Various proteins such as collagen, fibronectins, elastins, and laminins make up this vital matrix to aid and complete the process of wound closure. We see extracellular matrix damage mostly in our geriatric population … read more
The Whole Patient Approach
Addressing Common Comorbidities That Affect Wound Healing
When developing the plan of care for the patient with a chronic wound, it is imperative first to look at the “whole” patient and not just the “hole” in the patient.1 As we do, we are able to review any medical conditions or disease states that may affect wound repair and healing. Millions of Americans are affected by chronic wounds each year. These wounds include causes such as diabetic foot ulcers, venous leg ulcers, arterial insufficiency, and pressure ulcers. Common comorbid conditions that can affect healing include diabetes, venous insufficiency, peripheral arterial disease, cardiopulmonary and oxygen transport conditions, immune deficiencies, and dementia.2 This discussion is focused on these conditions and factors that contribute to chronic wounds and their management … read more
The Healing Trajectory: The Process of Wound Healing
There are four stages of wound healing. This systematic process moves in a linear direction. The four stages of wound healing are: hemostasis, inflammation, proliferation, and maturation. It is imperative to remember that wound healing is not linear. It is possible for a patient to move forward or backward through the wound healing phases due to intrinsic and extrinsic forces … read more
Current challenges and opportunities in wound care
3 CNOs weigh in
Wound care costs the U.S. healthcare system an estimated $50 billion annually. The large fiscal burden suggests wound care may be an overlooked target for quality improvement and cost reduction initiatives, according to Jacksonville, Fla.-based Healogics, the nation’s largest provider of advanced wound care services.
More than 30 million diabetics and 28.4 million individuals with heart disease reside in the U.S. Both morbidities represent public health epidemics and carry a heightened risk for chronic wound development. Approximately 6.7 million Americans are afflicted with chronic, non-healing wounds. This figure does not account for wounds attributable to conditions such as necrotizing fasciitis and surgical wounds related to the operating room. The Healogics team asserts that these numbers suggest America is experiencing a chronic wound epidemic.
On April 11, at Becker’s Hospital Review 9th Annual Meeting in Chicago, Arti Masturzo, MD, executive vice president of clinical innovation with Healogics, led a group of hospital leaders in a discussion on current challenges and opportunities related to wound care … read more
Fresh hypothermically stored amniotic allograft in …
the treatment of chronic nonhealing ulcers: a prospective case series
Introduction Millions suffer from diffcult to heal ulcers worldwide. The incidence of chronic ulcers is increasing rapidly, fueled by an aging population, rising incidence in obesity, diabetes, and venous insuffciency. Diabetic foot ulcers (DFUs), VLUs, and nonhealing postsurgical wounds are among the most frequently encountered ulcers in wound care practice. In the United States, over 4.3 million diabetic patients will develop a DFU in their lifetime, and ~2.5 million individuals suffer from VLUs. DFUs add 1–4 $9–$13 billion to the direct yearly cost associated with diabetes itself. The annual 5 cost of VLUs is $2.5–$3.5 billion. Nonhealing surgical wounds are also commonly 6 seen in wound care clinics. Surgical wounds pose an increased risk for infection and contribute to the growing economic burden of wound care management.
In recent years, several clinical trials have been conducted to investigate products derived from human amniotic membranes (HAMs) as adjunctive therapies to accelerate of different layers – the epithelium, basement membrane, and stroma – and these layers further consist of three contiguous but distinct layers – the inner compact layer, the middle fbroblast layer, and the outermost spongy layer. The HAM has been shown to have anti-infammatory, antifbrotic, antiangiogenic as well as antimicrobial properties. Research has confrmed that growth factors present in amniotic membranes can induce angiogenesis and human dermal fbroblast proliferation as well as recruit multiple stem cells relevant to wound repair and regeneration. 9,10
A fresh hypothermically stored amniotic allograft (HSAM) may improve healing rates by preserving growth factors and living cells, including stem cells, as well as retaining the membrane’s native structure. HSAM is aseptically processed and stored in a proprietary hypothermic storage solution using the Allofresh™ (Organogenesis, Canton, MA, sisting of topical antimicrobials. His comorbidities consisted USA) process. 13
Methods
A case study was conducted to evaluate an HSAM (Organogenesis) in the treatment of chronic wounds. Information was collected on patient demographics, wound type, wound location, age of wound, comorbidities, previous treatments, and current treatments. All patients were informed of study procedures and consented to have their case details and any accompanying photographs published. Digital planimetry (ARANZ Medical, Christchurch, New Zealand) was used ateach visit to record the wound surface area. Previous and current treatments were recorded. Two of the patients presented with VLU and one had a postsurgical wound.
The VLU patients had previously received compression, and one patient had also received negative pressure wound therapy. The one with a surgical wound had received a variety of previous therapies, including topical silver, Hydrofera Blue, and topical antibiotics. The age of the wounds for the VLUs were 2–3 weeks, while the surgical wound was 5 months. Comorbidities for the VLUs consisted of venous insuffciency, diabetes, arthritis, osteomyelitis to ulcer location, hypertension, and lymphedema. Comorbidities for the surgical wound patient consisted of arthritis and hypertension. The new treatment regimen consisted of HSAM covered with a knotted cellulose acetate fabric dressing (Adaptic ; Acelity, San Antonio, TX, USA) and appropriate standard of care, including offoading, multilayer compression, and of care, including offoading, multilayer compression, and surgical debridement.
Findings
Case 1
A 62-year-old patient presented to the wound clinic with a postop foot wound (nondiabetic), right foot dorsum. The duration of the wound was 5 months, with previous treatments consisting of topical antimicrobials. His comorbidities consisted of arthritis and hypertension. On day 0, the wound area size measured 3.3 cm , with 50% granulation, 10% fbrin, 40% slough, and a moderate amount of light red/pink serosanguineous drainage. Moderate edema was present. A 2.5 cm × 2.5 cm HSAM was applied and fxed in place using Steri-Strips™ (McKesson Medical-Surgical, Londonderry, NH, USA). On day 21, the wound area reduced to 2.9 cm2, a 12.12% reduction. There was an increase in the percentage of granulation tissue as well. By day 42, the wound area size had reduced by 81.82% with 100% granulation, and healed on day 71 (Figure 1).
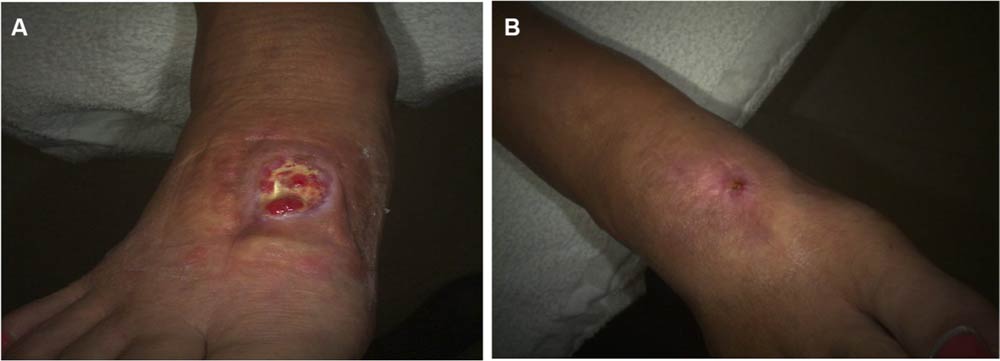
Figure 1 Case 1 surgical wound.
Note: (A) Day 0, 3.3 cm2 ; (B) day 71, 0 cm2.
Case 2
A 57-year-old patient presented with a left lower extremity VLU on the medial malleolus. The wound had been present for 8 weeks. The treatment thus far consisted of compression and topical antimicrobials. His past medical history included chronic venous insuffciency, peripheral vascular disease, deep vein thrombosis, and hyperlipidemia. On day 0, the wound area measured 0.3 cm . HSAM (2.5 cm x 2.5 cm) was applied and held in place with Steri-Strips™ ( McKesson Medical-Surgical) and compression wrap. On day 7, the wound was completed closed with no drainage (Figure 2).
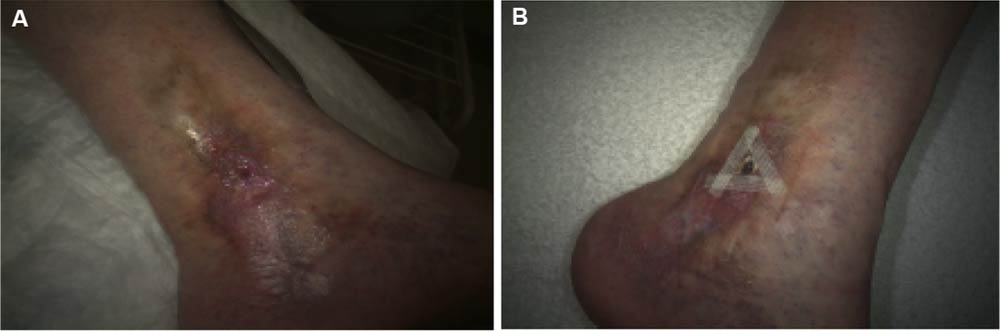
Figure 2 Case 2 venous leg ulcer.
Note: (A) Day 0, 0.3 cm2; (B) day 7, 0 cm2.
Case 3
A 70-year-old patient presented with a VLU on the medial right lower extremity. The wound had been present for 2 weeks. The medical history obtained from this patient revealed hypertension, lymphedema, type II diabetes, and chronic venous insuffciency. At the time of HSAM (2.5 cm × 2.5 cm) application, the wound area measured 1.0 cm . By day 7, the wound area was reduced to 0.4 cm , and by day 14, it achieved complete closure (Figure 3).
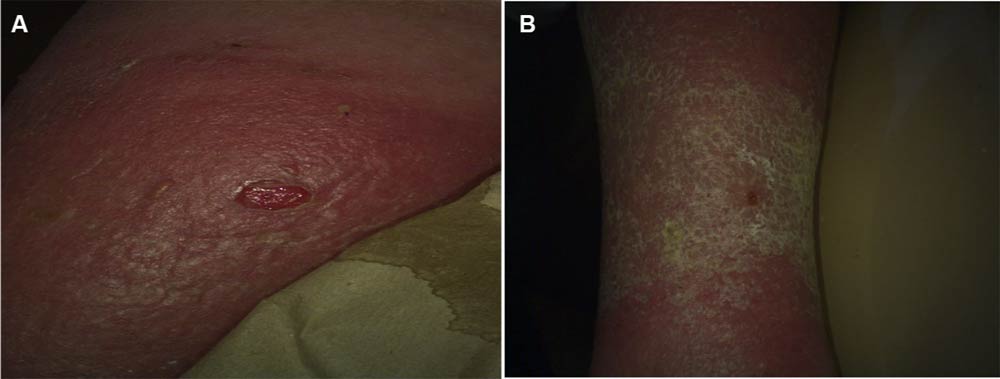
Figure 3 Case 3 venous leg ulcer.
Note: (A) Day 0, 1.0 cm2; (B) day 14, 0 cm2
Discussion
Prompt treatment of chronic ulcers is essential in preventing complications, reducing the cost of care, and lessening the economic burden on the health care system. In clinical studies, amniotic membranes have been shown to be effective in promoting healing in chronic wounds. Prior products consisted of dehydrated products. We postulated that fresh amniotic membrane would demonstrate even greater effect. Prior to embarking on large expensive clinical trials, we tried the fresh amniotic product on a few selected patients. Results from this study suggested that HSAM may be an effective treatment option for management of VLUs and other non-healing wounds. HSAM offers a new treatment alternative to promote healing in chronic wounds. This membrane contains numerous growth factors and cytokines. These growth factors are found to be released over an extended period and result in increased cellular migration, proliferation, and remodeling. Moreover, HSAM may reduce the long-term costs associated with the care of chronic ulcers by increasing the healing rate and lowering the risk of infection and complications This pilot case series was subsequently used to inform larger DFU and VLU trials that are ongoing at the time of this writing.
Complications in Chronic Wound Healing and
Associated Interventions
Overview of Chronic Wounds
Chronic non-healing wounds affect millions of patients each year and contribute significantly to their morbidity and mortality. These wounds have a substantial impact because of their economic burden and the significant effect on the reduction in quality of life, as well as the increased risk of death for those patients affected by them. A 2014 study of Medicare data showed that chronic non-healing wounds and associated complications affect nearly 15% or 8.2 million Medicare beneficiaries. The study also estimated the cost to treat these wounds at between $28.1 billion and $31.7 billion annually. The highest costs were associated with infected or reopened surgical wounds, and outpatient care had the highest site-of-service costs. In addition to being older, most of these patients have obesity and diabetes. Underlying causes often include diabetic foot ulcers, venous leg ulcers, arterial insufficiency, and pressure ulcers. The list of complications contributing not only to chronicity but also to further deterioration is quite lengthy.
Specific Wound Healing Complications and Interventions
The prevalence of chronic wounds and their complications has not been well documented in the literature. However underappreciated they may be, the complications associated with chronic wounds increase the cost—both financial and personal—to the individuals with these wounds.Although not an all-inclusive list, some of the more common complications include infection, tissue necrosis and gangrene, periwound dermatitis, periwound edema, osteomyelitis, hematomas, and dehiscence. Our purpose is to discuss the presentation of each and potential interventions … read more
The use of Prontosan® in combination with Askina® Calgitrol®
An independent case series
Many patients with chronic wounds will develop infection (Landis et al, 2007; Sibbald et al, 2011). Worldwide consensus on the specific use of silver antimicrobials recommends that silver dressings should be used initially for a ‘two-week challenge’ (Wounds International, 2012). Sixteen different individual case studies were carried out to evaluate the efficacy of a biofilm remover/cleanser in gel form, Prontosan® (B Braun), together with the use of an ionic releasing silver alginate, Askina® Calgitrol® Paste (B Braun) or Askina® Calgitrol® Thin (B Braun), when used on infected wounds. This study was completed in an advanced wound management centre in Pretoria, South Africa, during 2016. Selection criteria included wounds showing clinical signs of infection with delayed healing for more than 2 weeks. The study results showed that 50% of the wounds’ clinical signs of infection resolved within the 2-week antimicrobial challenge and by week 3, 81% of all clinical signs resolved. Ninety-three per cent of the wounds had improved wound progress and healing .. read more
Examining the Use of a Purified Collagen Matrix Plus PHMB Antimicrobial
Dr. Alisha Oropallo presents her poster, “Examining the Use of a Purified Collagen Matrix Plus Polyhexamethylene Biguanide Antimicrobial in the Management of Chronic Wounds,” which was exhibited as a poster at the 2017 SAWC Fall in Las Vegas, NV … view video
Managing inflammation by means of polymeric membrane dressings …
… in pressure ulcer prevention
Inflammation is the immediate normal response of the immune system to localised microscopic cell damage that precedes macroscopic tissue damage. Inflammation is triggered by secretion of chemokines that attract immune system cells to the sites of cell damage and facilitate their extravasation through increase in capillary permeability. The increased permeability of capillary walls in the inflammatory state consequently causes fluid leakage from the vasculature and, hence, oedema and associated pain. Polymeric membrane dressings (PolyMem®, Ferris Mfg. Corp.) are multifunctional dressings that focus and control the inflammation and oedema, and reduce pain. The literature reviewed in this article suggests that by having these effects on the inflammatory response, especially in fragile patients, the PolyMem dressing technology may facilitate repair of micro-damage in cell groups, which counteracts the evolution of damage to a macroscopic (tissue) level. Reducing the spread of inflammation and oedema in tissues appears to be a unique feature of PolyMem dressings, which supports repair of cell-scale damage under intact skin and tilts the delicate balance between the counteracting damage build-up and tissue repair mechanisms, thus promoting reversibility and self-healing … read more
Silver-impregnated Dressings for the Treatment of Chronic Wounds
A Scoping Review of the Use of Silver-impregnated Dressings for the Treatment of Chronic Wounds
Topical silver agents and dressings are used to control infection and promote healing in chronic wounds, but reviews published from 2006 to 2011 found heterogeneous results regarding their effectiveness. A scoping review was conducted to examine the extent, range, and nature of research activity surrounding chronic wound care that employed silver-impregnated dressings; identify research gaps in the existing literature; and summarize the evidence to provide recommendations for future clinical studies.
Ten (10) electronic databases and additional sources were screened from their inception to May 2016; search terms for the different databases included but were not limited to silver, chronic, complications, wound, ulcer, and sore. English-language articles that compared silver dressings with an alternate treatment in adults with chronic wounds and that reported clinical outcome measures were included. Of 222 full-text reviewed studies, 27 were included for qualitative analysis. Qualitative analysis was guided by key findings identified among the included studies that were analyzed in aggregate form where appropriate. In comparative analyses of the 26 studies that investigated wound healing … read more
Atypical Wounds: Causes and Management
Part 1 in a series discussing the etiology, assessment and management of atypical wounds.
As devoted clinicians to the field of wound management we take a responsibility to educate ourselves and others about wound etiologies and characteristics, as well as management of barriers to achieve positive outcomes. We spend a great deal of our careers learning about the most common offenders, such as pressure injuries, diabetic foot ulcers, venous stasis ulcers, arterial wounds, amputations, and traumatic wounds, to name a few. However, as our careers unfold we are faced with extra challenges, and atypical wounds are among them.
An atypical wound, also known as a wound of unknown etiology, is caused by a disease or condition that doesn’t cause a wound typically. Inflammatory diseases, infections, chronic illnesses, malignancies, or genetic disorders are examples of diseases that may result in the appearance of a wound. Atypical wounds can also arise from rare causes and usually share uncommon characteristics. In this two-part blog series, I discuss a few atypical wounds, to give you a view of this parallel universe … read more
Novel Approach to Chronic Wounds
Presentation on self-adaptive technology by Dr. Alex M. Reyzelman, the Co-Director of UCSF Center for Limb Preservation at RANDE 2015, International Wound Care Conference in Czech Republic.
Missouri university inventors have new creation to heal chronic wounds
ROLLA, Mo.–There’s a new way to heal chronic wounds that’s been invented in Missouri.
It’s a technique that inventors at Missouri University of Science and Technology are calling one of a kind.
The FDA approved the product called Mirragen and it uses bioactive glass to heal chronic wounds like people with diabetic foot ulcers and bed sores.
The inventors of the product told KOLR-TV of all the ways there are to heal chronic wounds, this is the most effective option for patients that they’ve seen.
Chad Lewis of ETS Wound Care says the bioactive glass product called Mirragen has received rave reviews …. read more
Biofilms and Inflammation in Chronic Wounds
Abstract
Significance
The incidence, cost, morbidity, and mortality associated with non-healing of chronic skin wounds are dramatic. With the increasing numbers of people with obesity, chronic medical conditions, and an increasing life expectancy, the healthcare cost of non-healing ulcers has recently been estimated at $25 billion annually in the United States. The role played by bacterial biofilm in chronic wounds has been emphasized in recent years, particularly in the context of the prolongation of the inflammatory phase of repair.
Recent Advances
Rapid high-throughput genomic approaches have revolutionized the ability to identify and quantify microbial organisms from wounds. Defining bacterial genomes and using genetic approaches to knock out specific bacterial functions, then studying bacterial survival on cutaneous wounds is a promising strategy for understanding which genes are essential for pathogenicity.
Critical Issues
When an animal sustains a cutaneous wound, understanding mechanisms involved in adaptations by bacteria and adaptations by the host in the struggle for survival is central to development of interventions that favor the host.
Future Directions
Characterization of microbiomes of clinically well characterized chronic human wounds is now under way. The use of in vivo models of biofilm-infected cutaneous wounds will permit the study of the mechanisms needed for biofilm formation, persistence, and potential synergistic interactions among bacteria. A more complete understanding of bacterial survival mechanisms and how microbes influence host repair mechanisms are likely to provide targets for chronic wound therapy.
Researchers are Creating an App to Track and Analyze Chronic Wounds
With a $1.6 million award from the National Institutes of Health, an interdisciplinary research team at Worcester Polytechnic Institute is developing a smartphone app that could lower healthcare costs and improve care.
An interdisciplinary team of researchers at Worcester Polytechnic Institute (WPI) has received a four-year, $1.6 million award from the National Institutes of Health (NIH) to develop a smartphone app that will allow patients and their caregivers to track and assess chronic wounds, helping lower costs associated with frequent doctor and hospital visits, and catching serious complications before they lead to expensive hospitalizations and life-altering amputations.
Emmanuel Agu, associate professor of computer science and coordinator of WPI’s Mobile Graphics Research Group, is the principal investigator for the project. Co-principal investigators include Diane Strong, a professor in WPI’s Foisie Business School, Bengisu Tulu, an associate professor in the Foisie Business School, and Peder Pedersen, a retired professor of electrical and computer engineering.
The app, which is in the early development stage, is being designed to be used by patients and caregivers, including visiting nurses, who need to regularly check the status of potentially dangerous wounds in the home environment. It will make patients more involved in their own care, cut down on unnecessary doctor visits, and issue alerts when an emergency trip to the doctor or hospital is necessary, Agu said.
A 2017 study found that chronic, nonhealing wounds affect 5.7 million people in the United States, or about 2 percent of the population, at an annual cost of $20 billion. The cost of just transporting chronic wound patients to medical visits is estimated at about $200 million per year. “This is a big problem,” said Agu. “Wounds, wound management, and amputations have a huge cost, both financially and physically, for the people who suffer from them, as well as for their families. I like to work on real problems that make a difference for people. Much of my research is in imaging and computer graphics. Wound management is a problem that imaging technology can help with.”
Patients or their caregivers will use the app to photograph chronic wounds with a smartphone. Machine learning algorithms built into the app will measure wound assessment metrics, including size, depth, and color, which indicate how the wound healing is progressing. The algorithms will compare the readings over time to determine if the wound is shrinking or expanding, or if there are other changes, like darkening tissue, that could indicate a growing infection or other complication. The app will also compute a healing score that tells the patient whether the wound is getting better, is unchanged, or is worsening. Finally, the app will suggest one of three actions: stay the course, consult a wound specialist for advice regarding treatment, or seek immediate care.
The new wound app is an evolution of work Agu and his research team completed for Sugar, an app designed to help people with diabetes track and manage their weight and blood sugar levels, and also photograph and assess the status of any chronic foot ulcers. In the current research, Agu will build on the wound assessment component of Sugar, which was developed with a $1.2 million grant awarded in 2011 by the National Science Foundation (NSF). And while Sugar focused exclusively on diabetic wounds on the feet and legs, the new app is expected to one day be expanded to assess a broader array of chronic wounds, including arterial, venous, and pressure ulcers, also known as bed sores.
Agu, Pedersen, and Clifford Lindsay, assistant professor of radiology at University of Massachusetts Medical School, will lead an effort to address one of the key technical challenges of the new project: processing imperfect smartphone photos taken by amateurs. Agu said his team understands that patients are likely to take photos from too far away or too close up, from an angle, or under poor lighting. He said shadows are particularly problematic for wound analysis, because they affect how the computer vision algorithm perceives the wound’s colors and depth.
To address this problem, the team will develop algorithms similar to those used in facial recognition software that can transform each image so it appears as if it was taken straight on, at the proper distance, and under ideal lighting conditions. They will use techniques from an area of computer science called computational photography. “Computational photography has been applied to natural images, like landscapes, but not in the medical domain,” Agu said. “This is cutting-edge research that we believe will produce a good solution to this problem.”
In addition to fixing the images, the research team will need to train their algorithms to properly assess and interpret them, work that will draw on the decision support expertise of Strong and Tulu. The team will expose their algorithms to hundreds of images of actual wounds taken, with patient consent, by Lindsay. Raymond Dunn ‘78, chief of plastic and reconstructive surgery at UMass Memorial, is a consultant to the project.
Agu and the team will feed the photos, along with wound care specialists’ expert assessments of the wounds and what kind of treatments they require, into the machine learning system so the app will “learn” how to analyze the wounds and calculate what care advice to give. Agu’s team will also test the algorithms on realistic simulated wounds they create with special 3D printers.
“This won’t replace doctor visits entirely, but it will augment those visits,” said Agu. “Patients or caregivers can check in anytime they want using this app and get more feedback than they do with occasional doctor visits. If people self-monitor, they are more likely to change their behavior, keep a closer eye on their wounds, and take the proper care those dangerous wounds need.”
The wound app is being developed on the Android platform, but Agu expects it ultimately to be adapted for the iPhone platform as well.
About Worcester Polytechnic Institute
Founded in 1865 in Worcester, Mass., WPI is one of the nation’s first engineering and technology universities. Its 14 academic departments offer more than 50 undergraduate and graduate degree programs in science, engineering, technology, business, the social sciences, and the humanities and arts, leading to bachelor’s, master’s and doctoral degrees. WPI’s talented faculty work with students on interdisciplinary research that seeks solutions to important and socially relevant problems in fields as diverse as the life sciences and bioengineering, energy, information security, materials processing, and robotics. Students also have the opportunity to make a difference to communities and organizations around the world through the university’s innovative Global Projects Program. There are more than 40 WPI project centers throughout the Americas, Africa, Asia-Pacific, and Europe.
Contact:
Alison Duffy, Director of Public Relations
Worcester Polytechnic Institute
Worcester, Massachusetts
508-340-5040, amduffy(at)wpi(dot)edu
For the original version on PRWeb visit: http://www.prweb.com/releases/2018/02/prweb15232174.htm
Wound Care Advantage Introduces the First Referral Source Algorithm in the …
SIERRA MADRE, Calif.–(BUSINESS WIRE)–The prevalence of chronic wounds in the U.S. now impacts 6.5* million people, similar to the number of individuals diagnosed with heart failure. To help its partners increase awareness of their wound care programs in local communities, Wound Care Advantage (WCA) has launched FlightPlan™, the industry’s first referral source algorithm. FlightPlan makes it easy to identify local physicians treating patients who may be in need of advanced wound treatment.
“We look for smart ways to develop and integrate technology into all areas of our organization,” said Nick Keezer, CTO of Wound Care Advantage. “FlightPlan was designed around three main objectives: to identify providers or physicians with patients who may need specialized care; to reduce the time it takes for a wound program to connect with the local community; and to better track and manage community education efforts.”
Finding local patients that need wound care, when they need it, can be a major challenge for wound center management … read more
UniSA research flying towards healing chronic wounds

Professor Allison Cowin, Research Professor, Future Industries Institute, University of South Australia
The same gene which enables flies to fly could hold the answer to healing chronic wounds.
Professor Allison Cowin is developing the world’s first human therapeutic antibody for the cytoskeletal protein Flii, also known as ‘Flightless I,’ which has been found to improve wound healing. This medical advancement is game-changing for the treatment of wounds and is particularly valuable for children with the debilitating rare skin condition epidermolysis bullosa (EB).
“Our initial experiments have found that Flightless I plays an important role in the development of the skin barrier and thickness – so our antibody has the potential to not only help wounds heal but also to prevent the skin from breaking down again,” Prof Cowin says.
The Flii protein was first discovered by geneticists studying fruit flies who found that by removing this particular protein flies could no longer fly – hence the name Flightless … read more
Altered macrophage phenotypes impair wound healing
One of the defining features of chronic wounds is their high levels of inflammation. Patients present with high levels of inflammation, around 80%, of cells at the wound margin being macrophages and with wound fluid laden with proinflammatory cytokines. The latter is in part responsible for preventing wound closure, along with the low levels of growth factors. In healthy acute wounds, two types of macrophages can be found: pro-inflammatory M1 macrophages and antiinflammatory M2 macrophages, with more M1 cells present early post-injury and M2 appearing later to regulate repair and wound closure. This pro-repair M2 phenotype, that secrete a range of mediators including growth factors that regulate re-vascularisation and closure of a wound, is lacking in chronic wounds, leading to excessive inflammation, enhanced degradation within the wound, reduced matrix deposition and lack of closure … read more
Inflammation in Chronic Wounds
Non-healing chronic wounds present a major biological, psychological, social, and financial burden on both individual patients and the broader health system. Pathologically extensive inflammation plays a major role in the disruption of the normal healing cascade. The causes of chronic wounds (venous, arterial, pressure, and diabetic ulcers) can be examined through a juxtaposition of normal healing and the rogue inflammatory response created by the common components within chronic wounds (ageing, hypoxia, ischaemia-reperfusion injury, and bacterial colonisation). Wound bed care through debridement, dressings, and antibiotics currently form the basic mode of treatment. Despite recent setbacks, pharmaceutical adjuncts form an interesting area of research.
The skin forms an important and effective barrier against the environment. It plays a vital role in protection against insults such as bacteria, xenobiotics and dehydration. When a cutaneous injury occurs, the body initiates a series of complex events to re-establish this protection. Wound healing can be roughly divided into four continuous and overlapping phases: (1) haemostasis; (2) an immediate inflammatory response defined by an infiltration of cytokine-releasing leukocytes with antimicrobial functions; (3) these cytokines kick off a proliferative phase where new epithelium, blood vessels, and extracellular matrix (ECM) are laid down; (4) over a period of weeks to months, the wound contracts as the ECM is remodelled [1]. These highly regulated cellular, humoral and molecular processes have been described as an orchestral performance—a potential flawless interplay can lead to perfect regeneration; however, human adult wounds undergo a repair process that leads to scarring, and, in some cases, non-healing chronic wounds …. read more
Reducing infection in chronic leg ulcers with an activated carbon cloth dressing
Chronic wounds are likely to have an increased bioburden, which in turn increases the risk of local infection. Indeed, infection is one of the most frequent complications of non-healing wounds, resulting in longer treatment times, increased risk of morbidity, greater resource use (of both dressings and nurse time) and, most importantly, a high personal cost to patients and their families (Cooper et al, 2014). While the ultimate aim is to treat the underlying wound, use of antimicrobial dressings is the cornerstone of the treatment of infected wounds. Most antimicrobial dressings work by killing the bacteria, and are indicated for use only when there are clear signs of increased bioburden and/or clinical signs of infections. As such, their use is assessed after 2 weeks, at which point it is advised that the clinician switches to another type of dressing if the wound is observed to be healing (Cooper et al, 2014) … read more
New technology for accelerated wound healing discovered
Researchers have found a new way of accelerating wound healing. The technology and the mode of action involves using lactic acid bacteria as vectors to produce and deliver a human chemokine on site in the wounds. The research group is the first in the world to have developed the concept for topical use and the technology could turn out to be disruptive to the field of biologic drugs … Researchers at Uppsala University and SLU have found a new way of accelerating wound healing. The technology and the mode of action method published in the highly ranked journal PNAS involves using lactic acid bacteria as vectors to produce and deliver a human chemokine on site in the wounds. The research group is the first in the world to have developed the concept for topical use and the technology could turn out to be disruptive to the field of biologic drugs … Treatment of large and chronic wounds are a high cost burden to the health care system since effective tools to accelerate healing are lacking. Wound care is today limited to mechanical debridement, use of different dressings and significant amounts of antibiotics preventing or treating wound infections. With the aging population, occurrence of chronic diseases such as diabetes and the alarming global spread of antibiotic resistance, a treatment that kick-starts and accelerates wound healing … read more
Topical gel containing blood pressure drugs shown effective in healing chronic wounds …
Topical Gel Made From Oral Blood Pressure Drugs Shown Effective in Healing Chronic Wounds in Test Animals
An international team of researchers led by Johns Hopkins has shown that a topical gel made from a class of common blood pressure pills that block inflammation pathways speeds the healing of chronic skin wounds in mice and pigs.
A report of the findings, published Oct. 16 in the Journal of Investigative Dermatology, marks efforts to seek approval from the U.S. Food and Drug Administration (FDA) to use the gel application in treatment-resistant skin wounds among diabetics and others, particularly older adults.
“The FDA has not issued any new drug approval for wound healing in the past 10 years,” says Peter Abadir, M.D., associate professor …. read more
Biofilm and Wound Healing
Composition of Biofilm
Biofilm is a complex microbial community containing self- and surface-attached microorganisms that are embedded in an extracellular polymeric substance.1,2 The extracellular polymeric substance is a primarily polysaccharide protective matrix synthesized and secreted by the microorganisms that attaches the biofilm firmly to a living or non-living surface. This protective covering does not allow the body’s immune system to recognize the presence of the microorganism; therefore, the bacteria evade an immune response, avoid detection by standard diagnostic techniques, and avoid destruction by standard treatments. Because of the tenacity of the attached biofilm, the microoganisms are able to resist physical forces, such shear, and are able to withstand nutrient and moisture deprivation, altered pH, and the impact of antibiotics and antiseptics. For the purposes of this discussion we break down the formation and actions of biofilms and discuss their impact on wound healing … read more